| |
 |

Gut-directed hypnosis is one of the most effective ways to help relieve all IBS symptoms! Results can last more than 5 years.

Now On Sale!
Most Popular Recently »
No More Imodium!
Cooking with Soluble Fiber?
|
 |
|
| |


Take 10% Off IBS Books, Hypnosis Programs, Stress Kits, DVDs, & More!
Use Promo Code TUMMYCARE10
Plus - New Child's IBS Hypnosis Program & The IBS Child's Kit!
|
|
April 6, 2010 ~ Scroll down for full newsletter or follow the links:
Ask Heather »
IBS Attack! See What The Brain-Gut Dysfunction Actually Looks Like
IBS Recipe »
Daffodil Bars - A Sweet Treat
Research & Press »
IBS Runs In Families
»
Avoid Red Meat & Dairy, Prevent Cancer
Special Events »
Special Canadian Tummy Fiber Price & Free Shipping!
Special Letter »
Nurse Speaks Out About GI Docs & What Really Helps IBS

|
|
Enjoy this week's newsletter!
~ Heather Van Vorous
|
Did a friend send you this newsletter? Sign up here for your own free subscription.
Researchers call gut-directed hypnotherapy a "cure" for IBS!
The Best Gut-Directed Self-Hypnosis Program for All IBS Symptoms
 
Gives an average 85% reduction of pain and bowel dysfunction symptoms.
Listen to IBS Audio Program 100 samples!

Daffodil Bars These pretty daffodil-yellow lemon bars are creamy, tart-sweet, rich, and delicious. They are also low fat, dairy-free, and have a great soluble fiber foundation from the Tummy Fiber, which makes them a safe splurge for an IBS dessert. I love to make these bars in the springtime and garnish the serving plate with fresh daffodils (just don't eat the flowers!)
Makes about 20 bars
Crust:
grated zest of one lemon (use the small hole side of a cheese grater)
1 C all-purpose white flour
1/4 C powdered sugar
3 T organic Earth Balance spread (or any non-hydrogenated vegetable shortening)
Preheat oven to 350F. In a small bowl, blend all crust ingredients with your finger tips until crumbly. Press mixture firmly into an 8x8" square baking pan that has been lightly sprayed with cooking oil. Bake for 15-20 minutes, until pale golden brown.
While crust is baking, make the filling:
2 T Acacia Tummy Fiber
1 T canola oil
4 organic egg whites
1 C sugar
2 T all-purpose white flour
zest of one lemon
4 T fresh lemon juice
1 T orange flower water (optional, but really delicious)
1/2 t baking powder
In a large bowl, whisk all ingredients gently but thoroughly. Pour filling over crust (crust can be hot from oven) and bake 18-22 minutes until golden brown. Cool on rack. Dust lightly with powdered sugar before serving if you like.
The perfect drink with these bars is a hot cup of Peppermint Tummy Tea!
Are you just learning how to eat for IBS? A little intimidated at the thought of special IBS recipes? Not quite sure just what makes these recipes special in the first place? Don't worry! Get Eating for IBS on sale and find the answers to all your questions.
~ Heather's Tummy Fiber ~
For the Dietary Management of Abdominal Pain, Diarrhea, &, Constipation

Certified Organic Acacia Senegal ~ Pure Soluble Fiber
The prebiotic fiber that relieves both diarrhea and constipation!
** Very Economical ** Only 4 cents per gram of fiber!
** 100% Acacia Senegal ** Never Low Grade Acacia Seyal
 Nurse Speaks Out About GI Docs & What Really Helps IBS
Nurse Speaks Out About GI Docs & What Really Helps IBS
Hi Heather,
I am an RN who works in a very busy GI practice, and almost 60% of my patients have IBS. I just want to let you know that years ago I had IBS - the worst.
I followed your books, The First Year: IBS and Eating for IBS, and your website, and believe it or not, after being faithful my body seems to have less and less attacks. Now, for the past few years, I can count on one hand how many I have had. I owe it all to you and your incredible knowledge about IBS.
I can't tell you how many of my patients with IBS are so frustrated and scared because they don't understand what is happening to them. Yes, they see the physician and get prescribed meds, and that seems to be about it, but then I take them aside and give them the name of your books and your website.
I encourage them all to get the books and follow them exactly as you advise. I then tell them my story and how after a while, they can look forward to the fact that the attacks may go away almost completely, or at least be controlled.
I have actually, finally, convinced many of the doctors in my practice to bring the patient to me when they are done, and let me speak to them about you. That took a while to happen. Doctors didn't seem to believe in it at first, but they seem to finally believe me now about your books.
A while back, doctors just thought IBS was only about controlling stress and it is so much more than that. They would leave the patients feeling just as lost as when they came in.
I feel like I am changing the way doctors (at least in my practice) just chuck it up to stress and say there is nothing to do for it. Mostly, that has come to pass due to all the calls I get from my patients thanking me for telling them about you, and then when they see the doctor, they tell him about our talk and how I gave them such great advice about you.
This is a good thing you are doing and I will spend the rest of my medical career telling my patients to buy The First Year: IBS and Eating for IBS and follow your advice to the letter.
I say this for myself and for the hundreds of my patients who have changed their lives and are now less frightened when they see their bellies bloat. They now understand why, and that they are not dying or have cancer, and that there is help out there for them that is more then just some pills to take. It is so much more than that.
I just wanted to thank you and let you know you are doing an amazing job.
Sandra
Thank you so much, Sandra! I am so thrilled by your letter! ~ Heather
Did you miss the recent letter from Erin, who no longer needs Imodium?
~ Heather's Tummy Tamers Peppermint Oil Capsules ~

Peppermint Oil Caps Called "Drug of Choice for IBS"
Our Peppermint Oil Caps have the added benefits of fennel and ginger oils, and they help prevent abdominal pain, gas, and bloating!
 IBS Does Run In Families
IBS Does Run In Families
A recent American Journal of Gastroenterology study found that people with IBS were three times as likely as people without the condition to have a relative who also had the disorder.
In the current study, half of the IBS patients' family members had symptoms themselves, compared to 27 percent of the control patients' families. This translated into a 2.75 times greater risk of IBS for patients' family members.
Researchers hope the findings will kick-start a hunt for genes that might be involved in IBS. Environmental factors shared within families could also be a factor.
While the findings have no treatment implications for people struggling with IBS right now, the researchers added, it may be reassuring for them to know that their symptoms have some biological cause.
Learn all about IBS and how to manage it with the essential guide, First Year IBS (now on sale!)
Go here for full article.
Avoid Red Meat & Dairy, Prevent Cancer
The Detroit News recently reported that avoiding red meat and dairy products is increasingly touted as helping to prevent cancer. A growing number of Metro Detroiters are embracing the idea so much they are taking classes to learn how to cook delicious yet simple meals without meat or dairy products such as milk, eggs, cheese, sour cream or yogurt.
They have good reason. A growing number of research studies on large groups of people indicate avoiding meat reduces the likelihood of battling cancer.
Last year, the National Cancer Institute released study results after examining 500,000 people for 10 years. The study concluded that eating large amounts of red and processed meats increased the likelihood of developing cancer. In the past few years, large studies in England and Germany showed that vegetarians were about 40 percent less likely to develop cancer compared to meat eaters.
Additionally, Harvard studies showed that daily meat eaters have approximately three times the colon cancer risk compared to those who rarely eat meat. Vegetarianism also is suggested for cancer survivors.
Learn how to eat well, manage IBS, and avoid red meat and dairy with Eating For IBS (on sale!)
Go here for full article.
  
Organic High Volatile Oil Fennel & Peppermint Tummy Tea Bags
Extraordinary Quality ~ Very Economical
Fennel is terrific for bloating & gas, Peppermint is great for IBS pain & spasms.
Heather's Fennel Tummy Tea Heather's Peppermint Tummy Tea
  
Compare for yourself! The pictures above show the huge difference in the quantity and quality of tea per teabag. The price comparison here is even more shocking!
 What A Brain-Gut Dysfunction Looks Like What A Brain-Gut Dysfunction Looks Like
Irritable Bowel Syndrome, as defined by the Rome Criteria diagnostic guidelines, is characterized as a brain-gut dysfunction. What on earth does this mean?
In plain English, it means that IBS symptoms result from a hypersensitivity of the nervous system of the gut, along with misinterpretations of the nervous system messages from the gut by the central nervous system and the brain.
Basically, this circuit (from gut to brain and brain to gut) appears to be abnormal in patients with Irritable Bowel Syndrome, though the exact abnormalities remain unclear.
Remarkably, PET scans of the brains of people with IBS show pronounced differences in the activation of certain parts of the brain relating to perception and pain (versus normal individuals). MRI brain scans have shown similar results.
This means that IBS is indisputably a physical problem. Simply put, the brain-gut interaction of people with IBS influences their bowel pain perception and motility. In a nutshell, the processing of pain information within the central nervous system varies between normal individuals and those of us with IBS, with the result that we can experience even normal GI contractions as painful.
The interactions between our brains, central nervous systems, and GI systems are just not functioning properly. We have colons that react to stimuli that do not affect normal colons, and our reactions are much more severe.
The end result is heightened pain sensitivity and abnormal gut motility, in the form of irregular or increased GI muscle contractions. It is this gut overreaction and altered pain perception that cause the lower abdominal cramping and accompanying diarrhea and/or constipation that characterize IBS.
However, while the underlying problem might well be in our brains, there is still a physical abnormality in the way our colons function. This dysfunction is actually visible (shockingly so) in the medical imaging tests below.
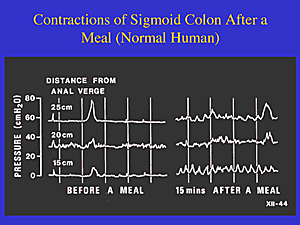
This is a normal gut 15 minutes after a meal.
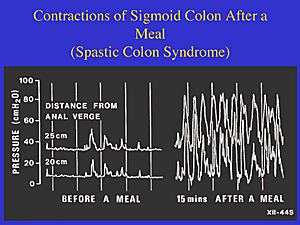
This is an IBS gut 15 minutes after a meal. Holy cow!
Illustration from Irritable Bowel Syndrome (IBS): Examining New Findings and Treatments. Authors: Marvin M. Schuster, MD; Michael D. Crowell, PhD; Nicholas J. Talley, MD, PhD. Continuing Medical Education Activity, Johns Hopkins School of Medicine, October 26, 2000, via Medscape. Used with permission.
Typically, the majority of the time the colon is still. However, following a meal, the stomach triggers something called the "gastrocolic reflex." This response occurs when food passes from the stomach into the upper part of the small intestine.
Normally, the gastrocolic reflex causes periodic contractions of the colon at different points along its length, at timed intervals. These segmented contractions regulate the flow of waste, and keep it in contact with the bowel wall, allowing water to be absorbed.
Finally, peristaltic contractions of the colon propel the waste to the rectum and then out of the anus via evacuation by a bowel movement. Total average transit time through the entire 30-foot digestive system, from mouth to anus, is between 12-24 hours for healthy individuals with high-fiber diets, and 48-72 hours for most Americans eating a typical Western (high fat/animal protein, low fiber) diet.
Where Things Go Wrong...
Unfortunately, how the digestive tract is supposed to work is not exactly how it does work for those of us with IBS. The key problem seems to be with the gastrocolic reflex. Specifically, research has found that many IBS patients have highly abnormal ones.
Our colons have disorganized and significantly more violent and prolonged contractions (leading to diarrhea), or almost no contractions at all (resulting in constipation).
Amazingly, researchers have found that while healthy people have between 6-8 peristaltic contractions in their colon within a 24-hour period, IBS sufferers with diarrhea have as many as 25 peristaltic contractions per day, and constipation-prone IBS patients have almost none.
Add to this bowel dysfunction the heightened pain perception resulting from our abnormal brain-gut interactions, and you've got the recipe for disaster...spelled I-B-S.
There's vivid demonstration of this in the images above. They show the huge difference between the after-meal contractions of a normal person's lower (sigmoid) colon and the contractions of the lower (sigmoid) colon in a person with IBS. The left half of both illustrations shows the colon contractions before a meal, and the rates are very similar and quite modest.
Just fifteen minutes after eating, however, the differences in colon contractions as shown on the right sides of the graphics are dramatic. Given the almost off-the-chart severity of the spasms (measured by the vertical axis in terms of pressure) in the IBS patient, it's easy to literally see exactly why the pain and bowel dysfunctions of this disorder can be so extreme.
As you read these graphics, don't be intimidated by the "distance from anal verge" legend for the horizontal axis of the chart. All that term basically means is how far up into the colon from the anus the contractions are being measured (they're either 15, 20, or 25 centimeters up into the colon from the outside of the anus).
In other words, the contractions triggered by the gastrocolic reflex from the stomach are affecting the very lower end of the colon just fifteen minutes after a meal has been eaten. This gives a crystal clear explanation for how an attack can hit you so fast and so hard after - or even while - eating.
Personally, I can't look at these charts without having flashbacks to all the times I've had to rush from the dinner table before I'd even finished my meal. The worst memory of all is from a vacation in Hawaii when I was twelve, and had been allowed to splurge and order lobster.
Unfortunately, a virgin pina colada (in hindsight, it was the high-fat coconut milk and high fructose pineapple juice on an empty stomach that did me in) triggered an attack before my meal had even arrived at the table. I spent the entire evening in a cold sweat vomiting from the pain in a bright pink hotel ladies lounge, while my family ate my lobster.
It's not much consolation to finally get a scientific explanation for exactly what happened to me that night, but I suppose it's nice to no longer be completely in the dark. (And I haven't had a pina colada since.)
No one really yet knows exactly why some people develop the brain-gut dysfunction of IBS and others don't. There is mounting evidence that for some IBS sufferers the condition is precipitated by some type of grievous insult to the gut - dysentery, food poisoning, intestinal flu, abdominal surgery, even pregnancy. The theory goes that even after full physical recovery from these traumatic events, the nerves within the gut retain a "memory" of the insult and remain hyper-sensitive to further stimulation, as well as prone to subsequent over-reaction.
You likely know if you experienced any abdominal trauma immediately prior to the onset of your IBS symptoms, and if you did it's probably nice to have a logical explanation for what has happened to your GI tract and why. There are those of us who are exceptions to this theory, however, who suffered no gut insult prior to the onset of IBS symptoms, and we're still patiently waiting for our explanation.
For full information about the brain-gut dysfunction and Irritable Bowel Syndrome overall, get The First Year: IBS, an essential guide to successfully managing the disorder. This is helpful for both the newly diagnosed and those who have been struggling with IBS for years.
Now that you know it's a brain-gut connection that's going wrong with your body, what can you do about it?
My top recommendation is gut-directed hypnotherapy. It's one of the most promising methods of treating IBS permanently (researchers have actually called it a cure!), and it deals specifically with the brain-gut dysfunction.
To manage symptoms on a daily basis, a prebiotic soluble fiber supplement can help regulate the gastrocolic reflex, and keep peristalsis normal. This can prevent abdominal spasms and cramps, and relieve both diarrhea and constipation.
~ Heather
Did you miss our recent "Ask Heather" and Cooking with Soluble Fiber?

Shop at Heather's Tummy Store for IBS
HelpForIBS.com
The only store that's just for IBS - so we only carry the very best
You're on this newsletter list because you have expressed interest in IBS news and information.
Change your newsletter email address here.
If you are viewing this newsletter on a website and would like to subscribe for email delivery, please "Join the IBS Newsletter" here.
ANTI-SPAM PRIVACY & SECURITY POLICY
HelpForIBS.com
Heather's Tummy Care
80 S. Washington St, #304
Seattle, WA 98104 USA
© 2010 Heather Van Vorous, Heather's Tummy Care. All rights reserved.
USA Copyright Office Registration Number TXU 1-270-858 and others.
|
|
| |